

If you’ve ever considered enhancing the shape or size of your breasts, you’re not alone. Breast augmentation is one of the most popular cosmetic surgeries in the United States. Whether you’re looking to add volume, restore symmetry, or feel more confident in your appearance, Dr. Sean Lille and his team in Scottsdale are here to help.
We believe every woman deserves to feel comfortable and beautiful in her own body. That’s why we provide expert care, honest guidance, and natural-looking results tailored to your unique goals.
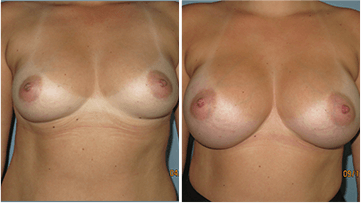
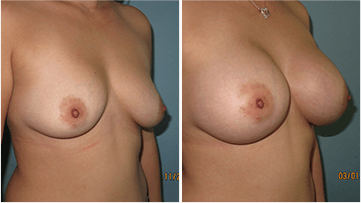
Breast augmentation, also called augmentation mammoplasty, is a surgical procedure designed to enhance the fullness and projection of the breasts. Most commonly, this is achieved through the placement of breast implants. Patients often seek this procedure for a variety of personal reasons, including restoring lost volume after pregnancy or weight loss, correcting asymmetry, or simply achieving a fuller appearance that better matches their overall figure.
This procedure can:
Each breast augmentation procedure is carefully customized. Dr. Lille works closely with every patient to determine the ideal implant size, shape, and placement to meet both aesthetic goals and lifestyle considerations. His priority is to create a look that is balanced and harmonious with the rest of the body.
There are many personal reasons why women choose breast augmentation. Some want to feel more feminine or confident in their appearance. Others simply want their clothes to fit better. Whatever the reason, our patients often tell us that the surgery gave them a boost in self-esteem and helped them feel more like themselves.
When planning for breast augmentation, one of the most important decisions is selecting the right type of implant. Patients typically choose between saline and silicone gel implants. Saline implants are filled with sterile salt water and are known for providing a firmer feel. In contrast, silicone gel implants are pre-filled with a cohesive gel that closely mimics the feel of natural breast tissue, making them a popular choice for those seeking a more realistic result.
In addition to implant material, Dr. Lille will discuss the implant profile. The placement of the implants is another key factor. Implants can be placed either above the chest muscle (subglandular) or below it (submuscular), with each method offering distinct advantages depending on a patient’s body type, activity level, and desired outcome.
The incision location is also chosen carefully to minimize visible scarring. Common incision sites include underneath the breast fold or around the areola. Dr. Lille uses advanced surgical techniques to ensure precise placement and natural-looking results.
Breast implants can be placed in one of two main positions:
Dr. Lille will discuss your body composition and help determine which placement is right for your goals.
Every breast augmentation journey begins with a private, one-on-one consultation with Dr. Sean Lille. He’ll take time to listen to your concerns, review your health history, and discuss your expectations. You’ll also:
Dr. Lille is known for his patient-focused approach. He will never pressure you into a decision. Instead, he’ll educate and support you so you feel empowered every step of the way.
Breast augmentation is performed under general anesthesia. After anesthesia is administered, Dr. Lille makes the agreed-upon incision and creates a space for the implant, known as the pocket. Once the implant is placed and positioned correctly, the incisions are closed with layered sutures to support optimal healing and minimize scarring.
Patients are monitored as they recover from anesthesia and are then sent home the same day with detailed post-operative instructions and a supportive garment to protect the surgical area and aid in the healing process.

The recovery process following breast augmentation is usually smooth and well-tolerated. Patients can expect some swelling, tightness, and soreness in the days following surgery. These symptoms are normal and typically subside within the first week. Many patients feel well enough to return to non-strenuous work after one week, though it is important to avoid heavy lifting or intense physical activity for at least three weeks after surgery.
Over the following months, the breasts continue to settle into their final position as the tissue adjusts around the implants. Dr. Lille provides comprehensive follow-up care to monitor healing and ensure that results are progressing as expected. By six weeks post-surgery, most patients have resumed normal routines and begin to enjoy the full benefits of their enhanced figure, although it can take three to four months for the implants to fully settle and “drop” into the pocket.
Breast augmentation is best suited for women who are in good overall health, have realistic expectations, and desire to improve the size, shape, or symmetry of their breasts. Whether the goal is to restore volume after pregnancy, balance body proportions, or simply feel more confident in clothing and swimwear, Dr. Lille helps each patient understand what the procedure can realistically achieve.
During the consultation, Dr. Lille conducts a full assessment and discusses all options in detail to help patients make an informed and comfortable decision.
“Dr. Lille is one of a kind! He is authentic and he is very reasonably priced considering his extreme experience, success record, and skill set. His staff is also very down-to-earth, smart, and experienced. He is lovable and truly cares about his connection to the patient, and treatment outcomes. (I’ve been working in healthcare and pay attention to these things). The office is pleasant and not a shiny opulent showcase (I’m uncomfortable with). I would trust my parents and kids in his hands too, in a split second. (Plus, he’s Navy, Special Forces man! Fun pictures while you’re waiting.) My implant ruptured and his replacement work made me look even better than my first surgeon years ago!”

Dr. Sean Lille is a board-certified plastic surgeon by the American Board of Plastic Surgery and a proud member of the American Society of Aesthetic Plastic Surgery. Recognized for his expertise, Dr. Lille serves as the ABC15 News Plastic Surgery Consultant for the Phoenix metropolitan area and has authored over 70 publications in leading plastic surgery journals.
Before establishing his private practice in Scottsdale in August 2000, Dr. Lille honed his skills at the prestigious Mayo Clinic, where he developed advanced surgical techniques and earned a reputation for excellence in patient care.
With extensive training and experience in a full range of aesthetic procedures, Dr. Lille is committed to helping each patient achieve their desired results. He has received thousands of glowing testimonials from patients who commend his exceptional skill, professionalism, and compassionate approach.

If you’re ready to feel more confident in your body, we’re here to help. Schedule your consultation today to meet with Dr. Sean Lille and begin your journey toward natural-looking, beautiful results.
📞 Call us at (480) 661-6197
📍 Visit us in Scottsdale, AZ
🌐 scottsdaleplasticsurgeon.com